Two UH engineering professors have developed novel optical probes with potential applications in improving diagnosis and treatment for patients with kidney disease. Exciting new results on the two probes were recently published in Biomedical Optics Express, the flagship journal of the Optical Society of America, and the Journal of Biophotonics, another top journal in this field published by Wiley.
Wei-Chuan Shih, assistant professor of electrical and computer engineering, and Chandra Mohan, Hugh Roy and Lillie Cranz Cullen Endowed Professor of biomedical engineering, began collaborating just over a year ago. Shih’s expertise is in molecular sensing using light-based sensing technologies such as optical probes. Mohan is a renowned expert on the genomics and proteomics of lupus and other autoimmune diseases, and the central goal of his research is to find new biomarkers and targets for treating autoimmune diseases.
Although their research interests may not appear so compatible at first glance, the two professors realized an ideal partnership in one another. Shih’s optical probes, which have been used for applications ranging from non-invasive glucose monitoring to detecting bacteria and sensing environmental hazards such as oil spills, can also function as a less invasive method of determining creatinine levels in patients with kidney disease.
One of the most common organs to be attacked by lupus is the kidney, manifesting in lupus nephritis. An estimated 40 percent of lupus patients develop this condition, which causes inflammation of the kidneys, impairing their ability to get rid of waste products and other toxins from the body effectively. Lupus nephritis is a leading cause of lupus-related deaths and results in tens of thousands of hospitalizations per year.
In order to track the kidney health of lupus patients, physicians must closely monitor the levels of creatinine, a chemical waste molecule, in the patients’ blood and urine streams. Creatinine is a fairly reliable indicator of impaired kidney function; as a patient’s kidneys become more impaired, the creatinine levels in the patient’s blood will increase.
“Currently, patients need to go into a doctor’s office or hospital to provide blood and urine samples. Doctors then use a chemical assay to determine creatinine levels in the patient’s blood and urine, and those are expensive and time consuming,” Mohan said.
“More importantly, a patient can’t assay these at home, for sure,” he added.
Shih’s optical probe, however, provides a cheaper, faster and less invasive alternative to drawing blood to monitor a patient’s creatinine levels. The probe is made up of a biochip integrated with a gold plasmonic nanostructure consisting of light-excited electrons. Plasmonics enables very strong light-matter interactions near the surface of these gold nanostructures, which Shih said will allow certain “hotspots” on the biochip to interact with nearby molecules. Shih’s group has developed novel highly porous gold nanoparticles with research results published in 12 journal papers and three pending patent applications over the past three years.
Based on how excited the electrons become – that is to say, how much they oscillate in response to a certain interaction – Shih is able to develop what he calls “fingerprints” of various molecules.
Because creatinine has a unique Raman scattering signal, Shih said the optical probes can detect creatinine levels with far higher sensitivity than the chemical assay tests that are currently used to quantify creatinine levels in urine or blood. Moreover, the probe only needs a tiny sample of urine – 5 microliters to be exact – to provide an accurate read of creatinine levels in a matter of seconds.
“The increased sensitivity of this probe in comparison to chemical assay tests could allow for earlier detection of renal impairment and therefore earlier intervention for patients with kidney diseases,” Mohan said.
The ultimate goal of this research, Mohan added, is to develop an optical probe that can be used to quantify creatinine levels in the blood and eventually even on the surface of the skin.
“So it’s more sensitive, cheaper and faster than the standard chemical assay test,” Mohan said. “But it’s not ready to be sold over-the-counter to be used by a patient in their own home yet. That’s the goal: to miniaturize the detection system so it can be used by patients in their home so they can monitor their creatinine levels as often as needed without having to go into a doctor’s office.”
Applications for the optical probe could be expanded to help diagnose other diseases beyond renal disease, Shih and Mohan said.
Shih and Mohan published this study as an open access paper, titled “Reagent- and separation-free measurements of urine creatinine concentration using stamping surface enhanced Raman scattering (S-SERS), in the January 2015 issue of Biomedical Optics Express.
To access the full article, please visit https://www.osapublishing.org/boe/abstract.cfm?uri=boe-6-3-849.
In another study, published in the Journal of Biophotonics, Shih and Mohan outline a novel method for using Raman spectroscopy to provide diagnostic information on kidney conditions and their severity.
Currently, physicians rely on an invasive procedure called a renal biopsy, or kidney puncture, to directly observe a patient’s kidney function. In addition to potential side effects, renal biopsies cannot be repeated serially because of the damage it causes to the kidney tissue. Shih and Mohan believe the optical probes they developed can offer a far less invasive alternative to replace kidney puncture procedures for diagnosing kidney disease.
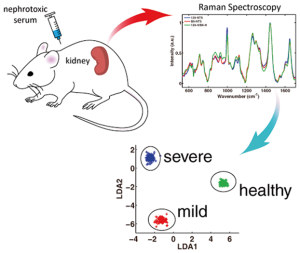
In this study, Shih and Mohan did not have a specific molecule or biomarker, such as creatinine, that they were looking to identify using Raman scattering. What they did have, however, was the knowledge that a diseased kidney and a healthy kidney give off two different Raman signals.
“There are some molecules that must be responsible for these different Raman signals, but we don’t need to know what those molecule may be. As long as there’s a difference in the signal, that’s good enough – you can easily differentiate between a diseased kidney’s Raman signal and a healthy kidney’s Raman signal,” Mohan said.
Using mouse models with induced kidney disease, Shih and Mohan were able to use the optical probe to differentiate between a healthy and a diseased kidney without puncturing the organ’s tissue. Shih’s research team developed a metric to broadly quantify the level of disease using the Raman scattering signals.
“We are proposing the nephrologist will puncture the patient’s skin, go to the surface of the kidney, and not puncture kidney, but probe the surface of the tissue and acquire Raman signals,” Mohan said. “The patient will feel a little pinch and poke through the skin, but the kidney is not hurt at all.”
The morbidity and mortality associated with the optical probe would be significantly less than the kidney puncture procedure. However, Shih and Mohan urged that more research is needed before the optical probe can replace the kidney biopsy for patients with renal disease.
“We hope that the Raman signals on the surface of the kidney is as good as a microscopic pathology, but we don’t know yet,” Mohan said. “The next step is to see if spontaneous models of lupus kidney disease can also be accurately diagnosed using the Raman probe.”
To access the full article, please visit https://onlinelibrary.wiley.com/doi/10.1002/jbio.201500109/abstract.